The death care profession is more than just dealing with dead bodies, and we want to educate you about all the different career options you have in this field.
For the latest instalment of our ongoing series, Careers in Death Care: A Day in the Life, we caught up with Aditi Sethi-Brown, MD to talk about what a hospice doctor does and how her work helps people peacefully die.
Aditi Sethi-Brown, MD is a Hospice and Palliative Medicine physician in Asheville, NC. She has spent the last 10 years working in an inpatient hospice setting and has a deep passion for work with the dying. She trained as a death doula and is co-founder of Center for Conscious Living and Dying, a collaboration with Cassie Barrett, a green cemetery operator. She is an Indian devotional and American folk musician. She lives in Black Mountain, NC with her husband, Jay, and their three precious children.
Careers in Death Care: A Day in the Life Series
♦ Careers in Death Care – Your Career Options
♦ A Day in the Life of an Aquamation Tech
♦ A Day in the Life of a Cremation technician
♦ A Day in the Life of a Gravestone Conservator
♦ A Day in the Life of a Death Doula
♦ A Day in the Life of an Embalmer
♦ A Day in the Life of a Forensic Artist
♦ A Day in the Life of a Funeral Director
♦ A Day in the Life of a Funeral Celebrant
♦ A Day in the Life of a Green Cemetery Director
♦ A Day in the Life of a Hospice Nurse
♦ A Day in the Life of a Hospice Physician
♦ A Day in the Life of a Pathologist
Careers in Death Care: A Day in the Life of a Hospice Physician

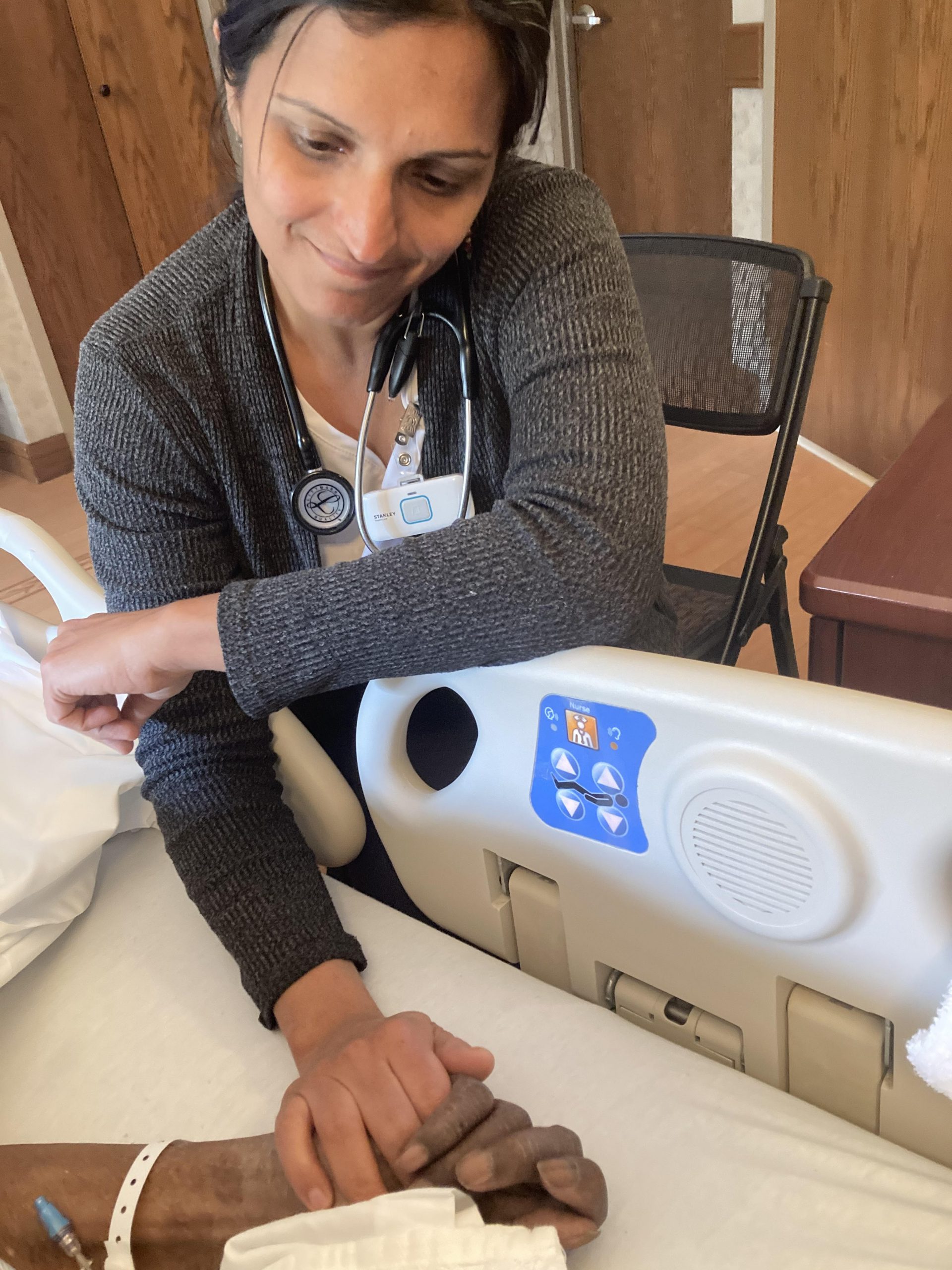
Image by Taylor Johnson
Tell us about yourself and what brought you to become a hospice physician?
When I was a young child, my parents sang me Hindi lullabies before tucking me in to bed. Their singing filled my heart with such love and tenderness. When they left the room, tears rolled down my face as I felt my separation from them, sensing the reality that they would not be around forever. So, from that time, I had an awareness of the transient nature of life.
Fast forward 13 years: When I was 17 and a freshman at Davidson College in North Carolina I began volunteering with Hospice. I had attended a volunteer fair for students where a lovely woman at a Hospice booth invited me over and told me about how Hospice serves individuals and their families when faced with a terminal illness. I enrolled in a training program and volunteered with Hospice throughout college.
Through supporting dying individuals and their families, I experienced how precious and meaningful time is in the presence of those facing their mortality. During a period in my life when I was insecure in many ways, I felt remarkably at ease with people contemplating profound realities about existence and reflecting on their lives–their fears, regrets, memorable moments, and legacies. I felt a deep knowing then that this would be my life’s work.
What inspired you to become a hospice physician?
 My parents are physicians who practice neurology, an area of medicine where observation, listening to individual stories and experiences and human connection are equally if not more important than ordering and analyzing labs and test results. Their passion and love of medicine influenced me as I reflected on how I wanted to be of service in the world. In college, I created a major through the Center for Interdisciplinary studies entitled “Religious Studies and Medical Humanities.” I have always been interested in what it means to be human and in the ways in which individuals find meaning and purpose in their existence.
My parents are physicians who practice neurology, an area of medicine where observation, listening to individual stories and experiences and human connection are equally if not more important than ordering and analyzing labs and test results. Their passion and love of medicine influenced me as I reflected on how I wanted to be of service in the world. In college, I created a major through the Center for Interdisciplinary studies entitled “Religious Studies and Medical Humanities.” I have always been interested in what it means to be human and in the ways in which individuals find meaning and purpose in their existence.
After my first year of medical school, I participated in an end-of-life care internship in Chicago. I learned so much about hospice and palliative care, which solidified my passion for the work. When I returned to medical school, I organized an “End-of-Life Care Week,” with lunch lectures, presentations and discussions to attempt to fill some of the gaps I noted in our medical education.
Around the same time, I experienced the deaths of some remarkable souls in my life who were part of my extended family. I witnessed how little death and dying were discussed openly in our community and how death was subconsciously considered a “failure” on many levels. Throughout the rest of my medical training, I witnessed so much fear around death, among providers and the families they cared for.
I completed a family practice residency, which I chose because of my love for the care of the whole person. I then undertook Hospice and Palliative Medicine Fellowship for a year to deepen my understanding and expand my skill set in this work. After completing that program as one of the first “Fellows,” I stayed on as an attending hospice physician in a 26-bed-inpatient hospice facility.
What is the biggest misconception about hospice physicians?
A misconception about hospice physicians is that we “dope” people up with morphine and hasten death by doing so. The reality is, we use various medications as needed to ensure an individual is as comfortable as they can be or want to be. We start with low doses of medications and gradually adjust if needed.
Run us through a typical day as a hospice physician.

The majority of Hospice physicians travel to the homes of Hospice patients, but I work in a 26-bed inpatient hospice center which is like a hospital for hospice patients. It serves individuals needing extra medical attention for a short period of time. I work with an interdisciplinary team which includes registered nurses, certified nursing assistants, a chaplain and a social worker.
After I get settled in the morning, the nurses and I connect to see if there are any immediate needs for patients and their families. If not, I read the medical records of individuals that are new to me and I look over their medication regimen to get a sense of what they are needing to relieve their symptoms.
Mid-morning we have an interdisciplinary team meeting where we review every patient and their family in the center. We review physical, mental, spiritual and emotional aspects of their care. After the team meeting, I generally visit individuals that need my attention. Throughout the day I check in with families, address questions and concerns, and support individuals and their loved ones as they navigate this major experience in their lives.
I spend time during my day documenting in the medical records the physical changes that I am observing and the medical interventions and changes made in the care plan for each individual. Not everyone who comes to the center dies there. Some individuals stabilize and are discharged, either to their home or to a nursing facility, and I oversee that process.
I also spend time doing administrative duties, paperwork, filling out death certificates, and attending various meetings. Some days I have the opportunity to share my knowledge and experience with medical students, residents or fellows in-training.
What was one of the hardest days you encountered as a hospice physician?
Sometimes dealing with family dynamics, various personalities, and various stages of acceptance among individuals dying and their loved ones can be challenging. Recently, I was involved in the care of a woman who was dying of heart failure. She accepted hospice care for the extra support in her home, but she never accepted the fact that she was dying. She ended up in our center for respite care and she continued to decline. As her body was cueing her in to the fact that she was dying, she insisted upon returning to the hospital for aggressive medical intervention.
Despite multiple conversations with her chaplain, social worker and her medical team, she revoked hospice and was transferred back to the hospital. That same night she had a massive heart attack and died while undergoing CPR. Our hospice team had to come to a place of acceptance of the fact that she died in a hospital setting, not surrounded by her loved ones in a calm and peaceful environment. That’s what we wanted for her. What she wanted was to keep living at all costs. If it was her time to leave the world, she wanted to try everything medically possible to keep her in it. She reminded me that this work is about supporting and educating individuals, while honoring their unique wishes for the final days and moments of their lives.
What was one of the most memorable days you’ve had as a hospice physician?
Pre-COVID, we could utilize a large common area, known as The Great Room, where there is a living room with a fireplace, a piano, family kitchen, and dining area. One memorable experience was celebrating the anniversary of a gentleman dying of metastatic lung cancer and his beloved wife of 60 years. We had a party, and my bandmates joined us for some music, food, love and celebration. This was the last time he was surrounded by all his family and friends, as he died shortly after the gathering.
What are some of the problems and tensions in the American hospice system, and how should these be addressed?
Hospice began as a grassroots movement that relied on community and family support. It has become more medicalized and there are gaps that need to be filled and can be filled by the death positive movement and by creative ways of caring for those aging and dying. I hope that existing hospice programs (both for-profit and non-profit entities) will prioritize individual and family well-being as they navigate the complexities of budgeting, staffing, and compliance with national regulations and guidelines.
What type of education or training do you need to become a hospice physician?
A medical degree, a medical license, experience as a practicing physician, and an interest in end-of-life care are all that are generally required. Most programs request some sort of certification in hospice and palliative medicine. Some programs have a preference for fellowship-trained, board-certified physicians, which means a physician has had an extra year or two training in Hospice and Palliative Medicine and has passed a national board exam.
What advice would you give to someone starting out working in hospice (as a physician, volunteer, or otherwise), or someone interested in doing so?
If you feel a calling for this work, I encourage you to look for opportunities at your local hospice to volunteer, look into end-of-life doula trainings, attend talks and webinars on death and dying, read blogs and books about different perspectives and aspects of death and dying, and consider attending workshops or trainings on the topics that interest you. You can also support your family and community as they deal with their own deaths or deaths of loved ones. Other suggestions are to make a practice of reflecting on and contemplating mortality, and cultivating compassion and quiet presence for yourself and for the people you love.
Careers in Death Care: A Day in the Life Series
♦ Careers in Death Care – Your Career Options
♦ A Day in the Life of an Aquamation Tech
♦ A Day in the Life of a Cremation technician
♦ A Day in the Life of a Gravestone Conservator
♦ A Day in the Life of a Death Doula
♦ A Day in the Life of an Embalmer
♦ A Day in the Life of a Forensic Artist
♦ A Day in the Life of a Funeral Director
♦ A Day in the Life of a Funeral Celebrant
♦ A Day in the Life of a Green Cemetery Director
♦ A Day in the Life of a Hospice Nurse
♦ A Day in the Life of a Hospice Physician
♦ A Day in the Life of a Pathologist
Do you currently work in the end-of-life industry? Would you like to be featured in a future Careers in Death Care: A Day in the Life article? Please contact us with your job title and tell us about your experience in the industry!





























Comments